Click the triangle below to listen to the podcast brief and access the transcript by clicking here.
What you need to know
A spinal cord injury can lead to bowel problems:
- You may have problems moving waste through your colon (or large intestine).
- You may pass a stool when you don’t want to, or a stool may be hard to pass.
- These problems can cause pain in your abdomen.
- When eating, you may feel full sooner than normal, or you may eat less than you usually do.
- Bowel problems can contribute to depression or anxiety. You may feel overly concerned about not being able to control bowel movements in public. You may not want to do things outside of your home.
A bowel program can help you to control bowel movements. Following a bowel program can help you to avoid other problems and perhaps bowel surgery.
Understanding your body
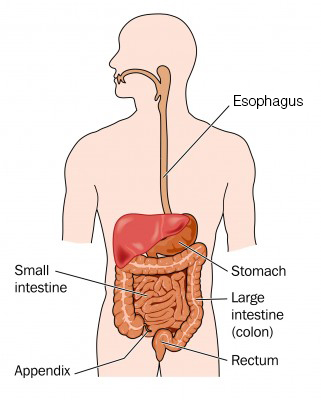
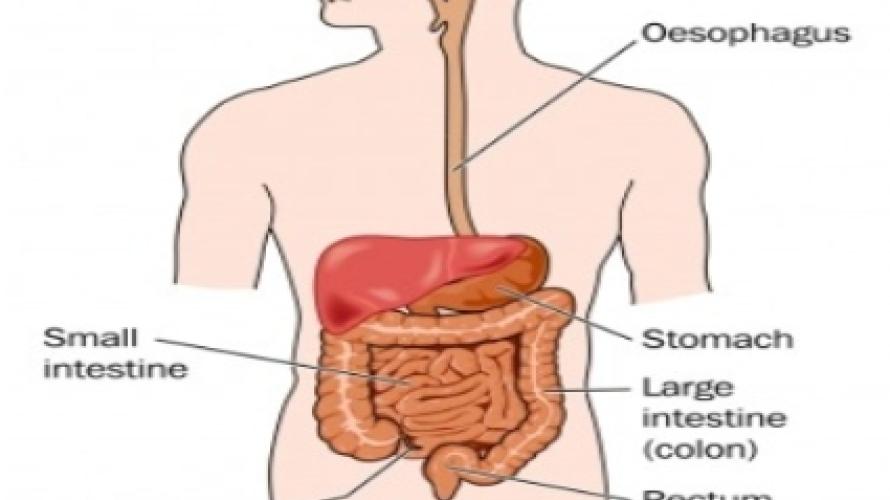
Your stomach and small intestine pull nutrients from the food you eat. Nutrients keep you strong and give you energy. The rest of the food becomes waste that your body doesn’t need. Waste forms into a stool in your colon and rectum and leaves your body through the anus. The process of passing a stool through and out of your body is known as a “bowel movement.” If you have a spinal cord injury, this process may be tough for you. For example, you may have a difficult time passing stools. This is called “constipation.” Or you may not be able to control when you pass a stool. This is called “stool incontinence.”
Spinal cord injuries may cause tightness (spasticity) or looseness (flaccidity) in the muscles of the rectum, sphincters, and pelvic floor. The degree of tightness or looseness may be related to the severity or completeness and level of your injury. If your injury is above level T11/T12, then the muscles of your sphincters and pelvic floor may be tight, which leads to constipation. If your injury is level T11/T12 or lower, then these muscles may be loose, which leads to stool incontinence. People with incomplete spinal cord injuries tend to have more muscle strength and sensation and therefore have fewer bowel problems than people with complete injuries.
What is a bowel program?
A bowel program is a plan to retrain your body to have regular bowel movements. A doctor or nurse designs a bowel program specifically for you. Your health, bowel and personal history, physical examination are an important part of this review:
- The level and completeness of your spinal cord injury
- Description and pattern of bowel problems
- Past and present medical problems
- Intake of food and drink
- Physical activities
- Need for or availability of resources
- Home environment
- Lifestyle
- Preferences
- Gastrointestinal tests
The goals of a bowel program are:
- Passing a stool on a daily or every-other-day basis
- Preventing unplanned bowel movements
- Emptying your bowel around the same time of day (e.g., morning, afternoon, or evening)
- Passing medium or large stool (about 2 cups) every time you have a bowel movement
- Emptying all or most of your rectum each day
- Having stools that are soft, formed, and bulky
- Emptying your bowel completely within 30 minutes (or 60 minutes, at most) after eating
What is involved in a bowel program?
A bowel program includes four parts: timing, diet (including food and fluids), medicines, and techniques to help with bowel movements. The program isn’t the same for everybody, because each person has different needs and responds differently to each part of the program.
Timing
A bowel program is best when done every day or every other day. A program involves:
- Eating a good diet and drinking plenty of fluids
- Using bowel medications, as recommended by your doctor
- Practicing techniques that activate the reflex to empty your rectum
- Using methods to clean out stools
Diet and fluids
Eating a good diet and drinking plenty of fluids are important to bowel health.
- Natural fiber from fruits and vegetables increases the bulk of stool, making it easier to move through the colon. Doctors recommend 38 grams of fiber per day for men and 25 grams per day for women.
- When eating a diet high in fiber, you should drink plenty of fluids. Water is best. You may get constipated if you don’t drink enough fluids. You should drink at least 2 or 3 quarts of fluids every day, unless told otherwise by your doctor.
- You should limit your intake of liquids with caffeine (e.g., coffee, tea, or energy drinks). These drinks actually remove fluids from your body.
Medicines
Your doctor may have you take one or more medicines, either orally or rectally:
- Stool softeners make stools soft and easy to move.
- Stimulant laxatives stimulate the colon to move stools.
- Bulking laxatives add shape and form to stools and prevent diarrhea (watery stools).
- Rectal laxatives help with rectal movement and emptying.
Some medicines may cause constipation. They may be ones that you’re taking already to reduce pain or muscle spasms or to treat depression. You may benefit from minimizing your use of these medicines under the supervision of your physician:
- Medicines to reduce pain, such as hydrocodone, oxycodone, morphine, fentanyl, gabapentin, pregabalin, or carbamazepine
- Medicines to treat bladder spasms but slow down intestinal motility, such as oxybutynin or tolerodine
- Medicines to stop muscle spasms all over the body, such as lioresal, tizanidine, or diazepam
- Medicines to treat depression, such as cymbalta, sertraline, or citalopram
Techniques
You can do one or more techniques to help you have a bowel movement and empty your rectum. You can do these at home or with help from a caregiver or nursing aid.
- Digital rectal stimulation—Move your fingertip in a small, gentle, circular motion around the rectum/anus. This motion stimulates reflex of the rectum/anus. Be sure to cut your fingernails short to avoid trauma. Perform this technique for 20 seconds and repeat it every 5–10 minutes until the bowel program is completed and the rectum is empty.
- Digital removal of stool: Use your finger to remove stool from the rectum. This will speed up your ability to empty the rectum.
- Enemas—Use a device to flush warm water into your rectum, which will help to empty it of stool. Examples of devices include the catheter enema or cone enema. If these simple enemas do not work, other home stool evacuation devices like the Peristeen enema and PIE (Pulsed Irrigation Evacuation) systems which have been approved by the U.S. Food and Drug Administration may help.
What if I am unable to do a bowel program or it doesn’t work?
A serious injury may keep some people from carrying out a bowel program. For others, the program just may not work. Every person is different. Surgery may be a good option in a few cases, for example:
- If you can’t achieve regular, complete bowel movements, which can lead to recurrent severe constipation (associated with frequent hospital admissions for stool loading and obstruction; chronic abdominal pain; prolonged [>1 hour], difficult bowel programs; or severe autonomic dysreflexia).
- If you have frequent stool incontinence (associated with pressure sores) or lack caregiver support, both of which may contribute to a poor quality of life and confinement in the home.
Other options include two kinds of surgery.
Colostomy
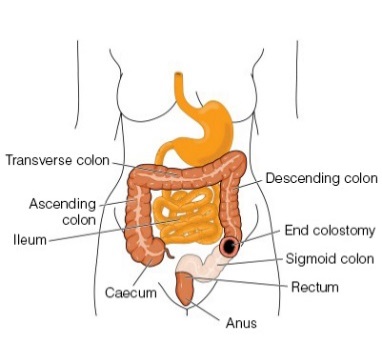
Surgeons attach the colon to the abdominal wall through a hole called a “stoma” (or opening). A bag is attached to the stoma. Stools pass into the bag instead of through the rectum. You or a caregiver empty and change the bag easily and regularly.
Most people who have the colostomy choose to have it permanently. The colostomy promotes good bowel movements and is easy to manage by yourself or by a caregiver. The procedure prevents stool incontinence and unplanned bowel movements. It also decreases mental stress so you can do more activities outside the home with family and friends.
Antegrade Continence Enema
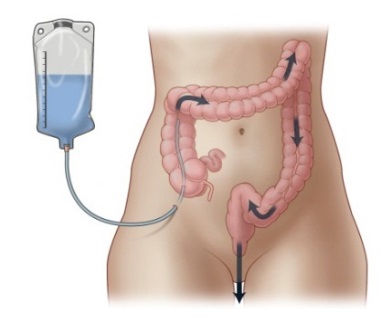
Surgeons open the abdominal wall to create a tract to either the first part of the colon (ascending colon) or the last part of the colon (descending colon/sigmoid) (See figure). You or a caregiver place an enema catheter through the stoma daily to flush the stool out of the colon with 500–1000mL of tap water. This process usually lasts from 30 to 60 minutes. Cleansing the colon daily and regularly prevents unplanned bowel movements and stool incontinence.
Why is maintaining bowel function so important?
Worsening and untreated bowel function can lead to many additional health problems:
- Partial paralysis of the stomach
- Chronic heartburn
- Gas pain
- Stomach or intestinal ulcers
- Hemorrhoids
- Abdominal discomfort,pain or distension
- Nausea
- Bloating or fullness
- Change in weight (related to a poor diet or a decrease in appetite)
- Autonomic dysreflexia - This is a serious condition where a dangerous elevation in blood pressure is associated with a drop in heart rate in people with spinal cord injury at levels T6 and above. It may cause heavy sweating, flushing, headaches, and blurry vision. If left untreated, it may lead to stroke, bleeding in the eyes, swelling of the heart or lungs, and other severe health problems.
- Worsening pain and/or spasticity
- Decreased sense of well being
These health problems can reduce your quality of life. But you may be able to avoid these problems by following a bowel program every day. Your doctor or nurse can help you and will check with you to see how you’re doing. Ask questions, and let your health care professional know about any problems you’re having.
Authorship
Bowel Function Problems After Spinal Cord Injury was developed by Gianna M. Rodriguez, M.D., in collaboration with the Model Systems Knowledge Translation Center.
Disclaimer
This information is not meant to replace the advice of a medical professional. You should consult your health care provider regarding specific medical concerns or treatment. The contents of this fact sheet were developed under a grant from the National Institute on Disability, Independent Living, and Rehabilitation Research (NIDILRR grant number 90DP0012-01-00). The contents of this fact sheet do not necessarily represent the policy of Department of Health and Human Services, and you should not assume endorsement by the Federal Government.
Neither SCI Model Systems, MSKTC, or NIDILRR has examined, reviewed, or tested any product or device cited in the factsheet. None of the parties involved make endorsement, representation, or warranty as to any product or device contained in this factsheet.
Copyright © 2015
Model Systems Knowledge Translation Center (MSKTC). May be reproduced and distributed freely with appropriate attribution. Prior permission must be obtained for inclusion in fee-based materials.